September is National Pain Awareness Month, spotlighting an issue worthy of every healthcare provider's attention. According to Dr. Dennis O'Leary, president of the Joint Commission on Accreditation of Healthcare Organizations (JCAHO), unrelieved pain slows patient recovery, increasing the burden for patients, their families, and the healthcare system.
How well are hospitals managing pain? According to Gallup's 2004 patient loyalty database, 68% of outpatient surgery patients, 55% of outpatient test and treatment patients, and 53% of inpatients say they are "very satisfied" that their pain was managed effectively. In each of the three areas, the percentages satisfied with their pain management are lower than those for overall satisfaction with the healthcare facility. And despite a strong focus on pain management in most healthcare systems, the numbers have not improved since 2002. The findings could be worse, but there is room for improvement, especially among inpatients.
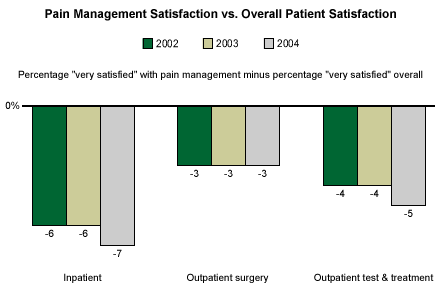
Why Hasn't Pain Management Improved?
Many patient care groups are focusing on pain management. Beginning in October 2005, the American Nursing Association will even begin offering pain management certifications. So, where are hospitals falling short?
Several years ago, I sat in on an emergency department meeting on pain management. One physician asked about the protocol for a sprained ankle, and other staff members said they don't medicate sprained ankles. This interaction illustrates an important point: Hospitals have made great progress in treating patients at the high end of the pain scale, but these patients make up a relatively small percentage of the overall population. Little is done to help patients suffering from less severe pain.
A case study of a mammography unit at one hospital provides another example. Mammography patients typically suffer only mild pain, but when looking at the patient satisfaction scores of this mammography unit compared with those of the hospital overall, pain management emerges as a key concern. Patients are told they will experience some discomfort during the procedure -- but one person's discomfort is another person's pain.
I'm not saying all patients suffering from mild pain should be medicated -- far from it. Much of the patient dissatisfaction in this area can be alleviated simply by ensuring that staff members are sensitive to situations in which patients are likely to experience discomfort. Most mammography patients obviously don't need to be medicated for pain -- but they do need care and compassion from staff members.
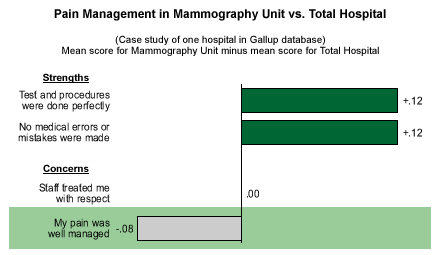
Many caregivers have become so focused on medicating pain that they have lost sight of the fact that most patients don't need pain medication, just old-fashioned TLC. Even among cancer patients, medication can go only so far. A caring nurse taking a little extra time to offer sympathy can make all the difference.
Bottom Line
JCAHO has published nine standards relating to pain management, which include ensuring staff competency in pain assessment and management, and establishing policies and procedures that support the appropriate prescribing or ordering of pain medications. (For the complete list, see the JCAHO link in Related Items.)
Hospitals should comply with these standards, but should not fall into a perceptual trap. Patients who score highly on the pain scale are not the only ones who need pain management, and caring and compassionate staff members are just as important to pain management as pharmacological solutions.