Healthcare issues, especially those relating to prescription drug coverage for the elderly, have been front-page news in many American newspapers over the past several months. At the heart of the issue is the question of how much responsibility the government should take for providing healthcare to its citizens, and how much of this responsibility should fall on the private sector. Is a two-tiered healthcare system -- in which the poor must rely on government-funded care (like Medicare and Medicaid), and the rich are able to buy more expensive (and perhaps higher quality) private sector health services -- acceptable? Gallup polling conducted in Canada and Great Britain -- two countries with universal healthcare access -- may offer some insight.
A Canadian Perspective
U.S. citizens are less concerned about healthcare than are their counterparts in Canada. In January 2001, 29% of Canadians identified healthcare issues as the most important problem facing their country, compared to only 7% of Americans who identified healthcare as the most important problem facing the United States. Is this discrepancy a result of structural differences between the two countries' healthcare systems? In the United States, reform advocates frequently voice concern about the country's health system becoming two-tiered. But interestingly, it seems that many Canadians already view the U.S. healthcare system as two-tiered, but don't necessarily see that as a bad thing.
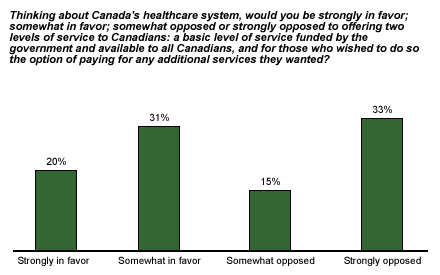
A March 2002 Canadian Gallup poll* asked Canadians if they would favor offering two levels of service in Canada: a free, basic level of service funded by the government; and for those who wanted it, the option of paying for additional services. A slim majority (51%) favored such a two-tiered system (20% strongly favored, 31% somewhat favored), while a slightly smaller percentage opposed it (15% somewhat opposed, 33% strongly opposed).
A British Perspective
The British press often criticizes the U.S. healthcare system, although capacity problems in the British National Health Service (NHS) have prompted some discussion about looking to the U.S. system as a model for improvement. A June 21 commentary in the British newspaper, The Guardian, criticized the U.S. system by noting that 40 million poor Americans (including 10 million children) are without health insurance, and that healthcare bills result in 40% of personal bankruptcies annually. The Guardian commentary concluded that importing the U.S. healthcare model to Britain would undermine the NHS.
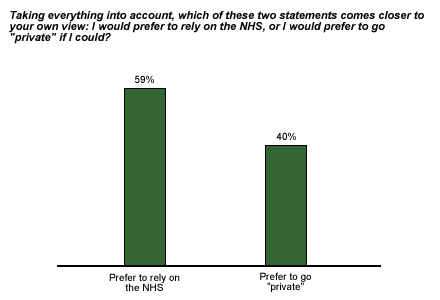
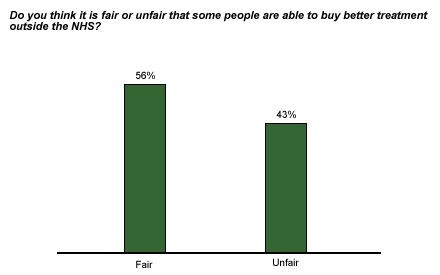
Yet in a December 2001 Gallup poll in Great Britain**, 46% of respondents said the NHS was in "somewhat failing health" and 19% described the health of NHS as "very poorly indeed." Would British citizens prefer a two-tiered health system? Forty percent of respondents said they would prefer to "go private" if they could, while 59% said they would prefer to rely on NHS. Additionally, 56% of British respondents said they think it's fair for some people to be able to buy better treatment outside of NHS.
Key Points
When examining options for improving access and quality and controlling costs, health policy researchers often look to the Canadian or British models. Yet the healthcare issue is as controversial in Canada and Great Britain as it is in the United States, if not more so. In the same way that U.S. experts may look to Canada and Great Britain for healthcare solutions, British and Canadian experts also look to the U.S. system.
A government-based safety net supplemented by private insurance for those willing and able to pay is actually a fairly apt description of the U.S. healthcare system. Admittedly, with healthcare access issues, lack of insurance coverage and the cost of prescription drugs, the safety net may have some significant holes in need of repair. But perhaps the reason that U.S. citizens are not more concerned about healthcare problems is because a two-tiered structure is more serviceable than reformers say it is. At least that's what some international perspectives seem to suggest.
*Results are based on 1,005 telephone interviews with Canadian adults, aged 18 and older, conducted March 12-18. For results based on the total sample, one can say with 95% confidence that the maximum margin of sampling error is ±3%.
**Results are based on 1,000 telephone interviews with British adults, aged 18 and older, conducted December 2001 to January 2002. For results based on the total sample, one can say with 95% confidence that the maximum margin of sampling error is ±3%.