Nothing in the world of living things is permanently fixed.
-- Hans Zinsser, Rats, Lice and History 1935
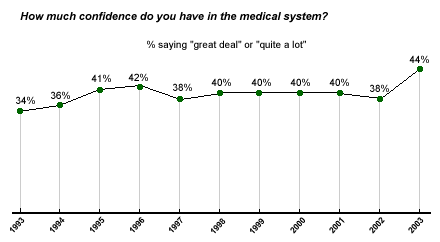
Recent Gallup Poll figures* indicate Americans' confidence in the U.S. medical system is up slightly over recent years. But lest healthcare officials decide this is a reason to celebrate, these numbers should come with a reality check. Despite recent rapid, high-profile advances in research and resulting clinical care, still only 44% of Americans have "a great deal" or "quite a lot" of confidence in the system, putting it in the middle of the 15 institutions tested, trailing the military, police, organized religion, and banks, among others. Perhaps most startling, 44% is the highest confidence rating Gallup has measured for the medical system since it began asking this question in 1993.
More specifically, one component of the medical system maintains abysmal confidence ratings. As previously noted in the Tuesday Briefing, only 17% of Americans have a great deal or quite a lot of confidence in HMOs.
It's logical to assume that this relatively low trust in the medical system could make Americans hesitant to use it. Given the benefits of prompt treatment for many ailments and the advantages of preventative care visits, this hesitancy could mean major problems for the medical system and society in general.
That Americans' confidence in today's medical system is not higher seems particularly ironic when the benefits of modern healthcare are put into historical context. People are living much longer, healthier, and more productive lives than they were a century, or even several decades, ago.
Of particular note is the control of infectious disease. Epidemics and pandemics have had devastating effects on the human population throughout history. Improved sanitation, improved nutrition, control of insects and rodents, and widespread use of antibiotics have largely brought infectious disease under control. Clinical progress continues: antiviral drugs now immunize people from chicken pox and influenza.
Even so, according to the U.S. Centers for Disease Control and Prevention, approximately 25% of physician visits are attributable to patients suffering from infectious disease. Emerging new infectious diseases such as HIV/AIDS and SARS, old diseases occurring in new geographical areas such as Hantavirus pulmonary syndrome, or known diseases re-emerging in antibiotic-resistant forms are real threats to Americans' well-being.
Confidence in the Medical System
Gallup research in numerous industries has confirmed that confidence is a crucial component of any decision to use a service or product. How might Americans' only moderate levels of confidence in the medical system affect the incidence and prevalence of infectious disease? Many may delay using the medical system as long as possible, or try alternative forms of treatment first, allowing illnesses to grow more serious. As we saw in the recent SARS outbreak, delays of any kind in the treatment process can have significant impact on transmission, resulting in increased morbidity and mortality.
Lower confidence ratings may also lead to fewer patients seeking preventative care, which defeats one of the purposes for which managed care programs were developed, and potentially costs the U.S. healthcare system billions of dollars as the avoidance of lower-cost preventative measures leads to greater incidence of expensive conditions such as heart disease.
Why Isn't Confidence in the Medical System Higher?
In Gallup's November 2002 Health and Healthcare survey**, 82% of Americans said that the overall quality of care they receive is good or excellent. When asked about the quality of healthcare nationwide, however, just 55% perceive it to be good or excellent. Furthermore, when asked about the cost of healthcare services in this country, 75% of Americans are dissatisfied.
Thus, Americans' moderate level of confidence in the medical system may have more to do with perceived and real costs than with the quality of care they actually receive.
Bottom Line
Given the costs associated with infectious disease and the failure to provide regular preventative care, the government would be well-advised to do whatever it can to improve the standing of the U.S. medical system in the eyes of Americans. Early healthcare interventions -- with low margins but high rates of return in terms of public health -- have not been successfully implemented.
Government promotion of affordable healthcare, focused explicitly on preventative care, would probably do much to increase the confidence of the American public in our medical system.
*Results are based on telephone interviews with 1,029 national adults, aged 18 and older, conducted June 9-10, 2003. For results based on the total sample of national adults, one can say with 95% confidence that the margin of sampling error is ±3 percentage points.
**Results are based on telephone interviews with 1,001 national adults, aged 18 and older, conducted Nov. 11-14, 2002. For results based on the total sample of national adults, one can say with 95% confidence that the maximum margin of sampling error is ±3 percentage points.